The Weight Loss Revolution: What You Need to Know About GLP-1 Medications and Modern Weight Management
Explore the science behind GLP-1 medications like Wegovy and Ozempic, and how they are changing the conversation around obesity, weight loss, and metabolic health.
Written by: Health Focus Research Team Medically Reviewed by: Dr. Priya Sharma, MBBS, MD – Board-Certified Endocrinologist & Obesity Medicine Specialist Last updated: February 28, 2026 | Reading time: 8 minutes
⚠️ Medical Disclaimer: This article is for informational purposes only. If you have metabolic conditions including diabetes, prediabetes, or insulin resistance, always consult your endocrinologist or physician before making dietary changes.
Weight loss has always been a charged topic—wrapped up in morality, willpower, and often shame. But something significant is shifting in how we approach weight management. A new class of medications is changing not just treatment options, but the entire conversation around obesity, health, and body weight.
If you’ve heard friends mentioning Wegovy, Ozempic, or Mounjaro, or noticed celebrities looking dramatically different, you’re witnessing what might be the most significant development in weight management since… well, ever. But beyond the headlines and social media buzz, what’s really happening here?
The Science Behind the Breakthrough
GLP-1 medications aren’t actually new—they’ve been used for diabetes management for years. What’s new is recognizing their profound effect on weight loss and their approval for treating obesity.
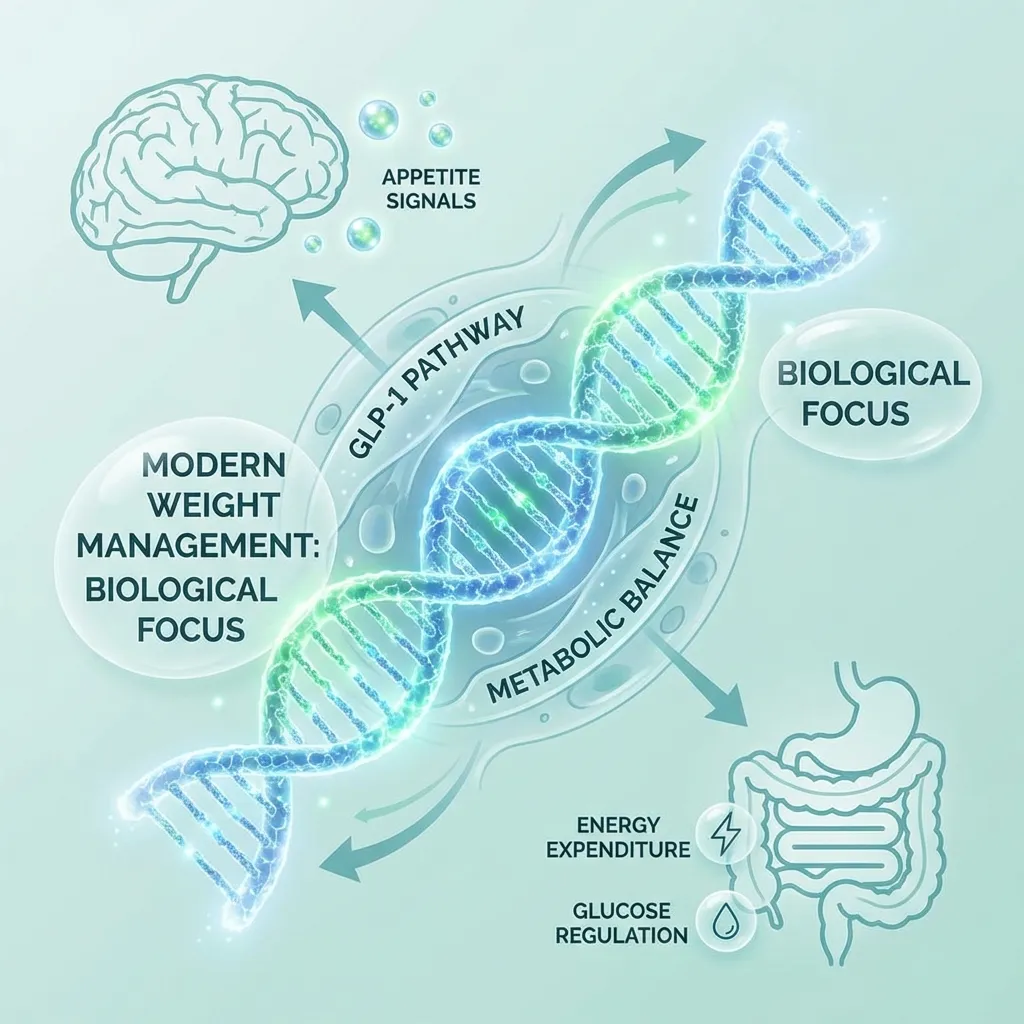
These medications (technically called GLP-1 receptor agonists) work by mimicking a hormone your body naturally produces after eating. This hormone does several things: it slows down how quickly food leaves your stomach, reduces appetite by affecting brain circuits involved in hunger and satiety, and helps regulate blood sugar.
The results have been nothing short of remarkable. In clinical trials, people taking these medications lost an average of 15-20% of their body weight—far exceeding what’s typically achieved through diet and exercise alone. Some of the newer medications in development are showing even more impressive results, with average weight losses approaching 25%.
But here’s what makes this particularly significant: for the first time, we have medications that appear to address the biological mechanisms underlying obesity, not just symptoms.
Why This Changes Everything
For decades, weight loss advice has been frustratingly simple: eat less, move more. The underlying assumption was that obesity was primarily a willpower problem—if you just tried hard enough, you could lose weight and keep it off.
We now know this is scientifically wrong. Obesity is a complex medical condition influenced by genetics, hormones, metabolism, brain chemistry, gut microbiome composition, environmental factors, and yes, behavior—but not simply a lack of willpower.
When people lose weight through traditional dieting, their bodies fight back. Metabolism slows down, hunger hormones increase, and satiety hormones decrease. Your body literally works against you to regain the lost weight. This is why so many diets fail—not because people lack discipline, but because they’re fighting powerful biological systems designed to maintain weight.
GLP-1 medications appear to work with these systems rather than against them. They’re not appetite suppressants in the traditional sense—they’re affecting the fundamental signaling that regulates hunger, fullness, and food reward in the brain.
The Reality Beyond the Hype
While these medications are genuinely groundbreaking, they’re not magic pills. There are important realities everyone considering them should understand.
Side effects are real: The most common side effects are gastrointestinal—nausea, vomiting, diarrhea, and constipation. For most people, these improve over time, but for some, they’re severe enough to stop treatment. There are also less common but more serious potential side effects that need medical monitoring.
They require long-term commitment: These aren’t medications you take for a few months and then stop. When people discontinue GLP-1 medications, they typically regain much of the lost weight. For many, this means committing to lifelong treatment—with all the cost, inconvenience, and potential unknowns that entails.
Cost and access are major barriers: These medications are expensive—often $1,000 or more per month without insurance coverage. While insurance coverage is improving, many plans still don’t cover weight loss medications, viewing them as “lifestyle” drugs rather than medical necessity.
They’re not for everyone: These medications work best for people with obesity or those with weight-related health conditions. They’re not appropriate for people who want to lose 10-15 pounds for aesthetic reasons. They also aren’t suitable for people with certain medical conditions or those who are pregnant or planning pregnancy.
Beyond Medication: The Bigger Picture of Weight Management
What’s fascinating about the GLP-1 revolution is how it’s changing the broader conversation about weight management. More people are recognizing that maintaining a healthy weight isn’t just about diet and exercise—it involves sleep quality, stress management, gut health, metabolic function, and yes, for some people, medication.
Sleep matters more than we thought: Poor sleep disrupts hunger hormones, increases cravings for high-calorie foods, and impairs the body’s ability to regulate blood sugar. People trying to manage their weight need to prioritize sleep as much as nutrition.
Stress and cortisol play major roles: Chronic stress promotes weight gain, particularly around the abdomen, through complex hormonal pathways. Stress also drives emotional eating and disrupts sleep—creating a vicious cycle.
The gut microbiome influences weight: Your gut bacteria affect how you extract calories from food, regulate appetite hormones, and even influence food cravings. People with obesity often have different microbiome compositions than those at healthy weights.
Protein is having a moment: There’s growing recognition that protein intake—not just calories—plays a crucial role in weight management. Protein increases satiety, preserves muscle during weight loss, and has a higher thermic effect than other macronutrients.
The Functional Nutrition Approach
Alongside medication advances, there’s a parallel movement toward functional nutrition—personalized approaches that consider individual metabolism, genetics, and health markers rather than applying generic advice.
This includes strategies like:
Metabolic testing: Understanding your personal glucose responses to different foods through continuous glucose monitors can reveal which foods spike your blood sugar and drive hunger and cravings.
Food timing: When you eat might matter as much as what you eat. Time-restricted eating (eating within a consistent daily window) can improve metabolic health independent of calorie restriction.
Nutrient density: Focusing on whole, minimally processed foods that provide maximum nutrition per calorie helps address nutrient deficiencies that can drive continued hunger even when calorie needs are met.
Individual responses: Recognizing that the “best” diet is the one that works for your biology, preferences, and lifestyle—not the one that’s currently trending.
The Mental Health Connection Nobody Talks About
One aspect of the GLP-1 conversation that deserves more attention is mental health. Food often serves functions beyond nutrition—comfort, stress relief, social connection, emotional regulation. When appetite is suddenly reduced or food loses its appeal (a common effect of these medications), people sometimes struggle psychologically.
Some report feeling a loss of pleasure or comfort they previously derived from eating. Others find that removing food as a coping mechanism exposes underlying anxiety, depression, or emotional issues they were unknowingly managing through eating.
This is why comprehensive weight management should include mental health support. Whether someone is using medication or not, addressing the emotional and psychological aspects of eating is crucial for long-term success.
What the Future Holds
The weight management landscape is evolving rapidly. Beyond GLP-1 medications, researchers are exploring:
Combination therapies: Medications that target multiple pathways simultaneously might be even more effective than current options.
Longer-acting formulations: New versions that require less frequent dosing (monthly or even quarterly injections) are in development.
Oral medications: The recent FDA approval of oral semaglutide (Wegovy tablets) is just the beginning. More convenient oral formulations are coming.
Predictive tools: AI and genetic testing might eventually help identify which treatments will work best for which individuals, moving away from trial-and-error approaches.
Making Informed Decisions
If you’re considering weight loss medications, here’s what matters:
Work with knowledgeable providers: This isn’t an area for quick online prescriptions without comprehensive evaluation. You need providers who will monitor your health, adjust dosing appropriately, and address side effects.
Consider your motivation: Are you pursuing weight loss for health reasons (diabetes risk, heart disease, joint problems) or primarily aesthetic reasons? The strength of medical indication matters for both decision-making and insurance coverage.
Understand the commitment: These medications work best as part of comprehensive lifestyle changes, not as replacements for healthy habits. You still need to address nutrition, activity, sleep, and stress management.
Be realistic about costs: If insurance doesn’t cover the medication, are you prepared for long-term out-of-pocket expenses? Some people start treatment only to discover they can’t sustain the cost.
Focus on health, not just weight: The most important outcomes aren’t the numbers on the scale—they’re improvements in metabolic health markers, quality of life, and reduction in disease risk.
The Bottom Line
We’re living through a genuine paradigm shift in weight management. For the first time, we have tools that work with our biology rather than demanding we fight against it. But these tools—whether medications or personalized nutrition strategies—work best when combined with lifestyle factors that support overall health.
More than anything, this revolution is helping destigmatize obesity and recognize it as the complex medical condition it is. Weight isn’t a moral issue. It’s not about willpower or laziness. It’s about biology, environment, genetics, and multiple interacting systems that we’re only beginning to fully understand.
Whether medication is part of your journey or not, the goal should always be the same: achieving and maintaining a weight that supports your health, wellbeing, and quality of life—in whatever way works for your unique body and circumstances.
Read Next
GLP-1 Drugs Are Changing Everything—Not Just Your Waistline
Ozempic and its cousins are being called the most important drugs since statins. But the story goes far beyond weight loss. Here's what GLP-1 drugs can treat, the risks nobody mentions, and what the revolution means for you.
Feb 16
Cold Plunges and Saunas: The Science Behind the Hottest (and Coldest) Wellness Trend
Is contrast therapy just a fad? Dive into the science behind cold plunges and saunas, and learn how temperature extremes can boost resilience, recovery, and longevity.
Jan 19
The Longevity Revolution: Why Living to 100 Is Just the Beginning
Discover why 2025 is the year aging stops being theoretical. From mitochondrial breakthroughs to longevity clinics, learn how to add not just years to your life, but life to your years.
Jan 19